Do natural variations in hormones, such as oestrogen, make anxiety disorders more likely? If so does this affect the way people respond to treatment?
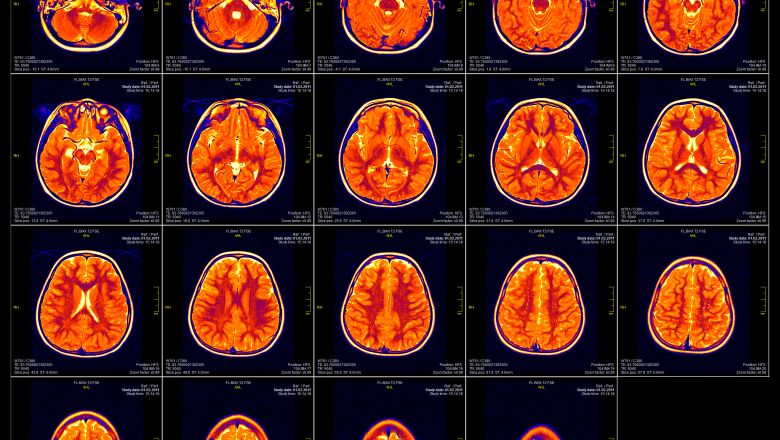
Hot spots of disease: The human connectome as a biomarker for brain disorders
Can patterns in the brain show the differences between mental health conditions – and speed up diagnosis and treatment?
The project
Many mental health conditions share similar symptoms, which can be a big barrier to quick, accurate diagnosis.
People are left waiting for a condition to be identified or are misdiagnosed. In both cases, the wait for effective treatment can be a long one.
So Martijn and his team are taking a fresh approach to analysing the similarities and differences between mental health conditions.
The process
By mapping activity between different areas of the brain in various mental health conditions, our researchers are hoping to identify patterns that are specific to single conditions and others that overlap.
That new knowledge would help to improve diagnosis, as well as increasing understanding of shared symptoms common to multiple mental health problems.
The potential
This project involves a new approach to understanding the similarities and differences between mental health conditions.
Advances in this area are vital if we are to accurately understand the nature of different conditions, and so inspire better diagnoses, better treatment and better outcomes.

Dr Martijn van der Heuvel works at the UMC Utrecht Brain Centre Rudolf Magnus in the Netherlands. He focuses on providing new insight into the rules that drive structural and functional brain networks.
Was this information helpful?
Related research profiles
Sensitive periods for the effects of depression on suicide risk: a longitudinal study of gene-environment interactions and epigenetic mechanisms
Dr Lussier aims to determine the extent to which child and adolescent depression interacts with genetic susceptibility to influence suicide risk in early adulthood.
Increasing access to social prescribing for people living with severe mental illnesses at risk of cardiovascular disease
People with severe mental illnesses are at high risk of heart disease due to lack of physical activity and social isolation. Social prescribing can help, but is it accessible?


